MCL Tear & Reconstruction
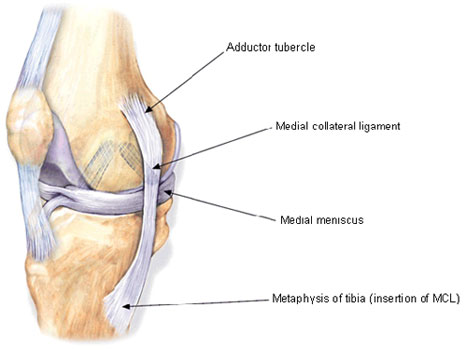
The Medial Collateral Ligament (MCL or Tibial Collateral Ligament) is one of the four major ligaments of the Knee. It is on the medial (inner) side of the Knee Joint in humans.
It is a broad, flat, membranous band, situated on the medial side of the Knee Joint. It is attached above to the medial epicondyle of femur and below to the medial condyle of tibia and medial surface of its body. It resists forces that would push the Knee medially (inwards), which would otherwise produce valgus deformity.
The ligament is divided into superficial and deep parts.

Tear of Medial Collateral Ligament:
Medial Collateral Ligament (MCL) Injuries are usually caused by contact on the outside of the Knee and are accompanied by sharp pain inside the Knee. Being fairly large and vascular the Medial Collateral Ligament has an excellent ability to heal. It is however important to recognize & treat acute medial complex laxity as early as possible. NSAID and the long hinged Knee brace are very helpful in the early physiotherapy and walking with full weight-bearing is allowed.
Grades of Tear:
- Grade I MCL
This is an incomplete tear of the MCL. The tendon is still in continuity, and the symptoms are usually minimal. Patients usually complain of pain with pressure on the MCL, and may be able to return to their sport very quickly. Most athletes miss 1-2 weeks of play.
- Grade II MCL
Tear Grade II injuries are also considered incomplete tears or Medial Collateral Ligament Injuries. These patients may complain of instability when attempting to cut or pivot. The pain and swelling is more significant, and usually a period of 3-4 weeks of rest is necessary.
- Grade III MCL Tear
A grade III injury is a complete tear of the MCL. Patients have significant knee joint pain and swelling, and often have difficulty bending the Knee. Instability or giving out is a common finding with grade III MCL Tears. A Knee brace or a Knee immobilizer is usually needed for comfort, and healing may take 10-12 weeks.
Signs & Symptoms:
Symptoms depend on the severity of the Medial Collateral Ligament Injury and are classified according to the extent of the injury. MCL injuries are classified as grade 1, grade 2 or grade 3. knee joint pain.
- Tenderness to touch
- Swelling, stiffness
- Internal bleeding (grade 2)
- Somewhat unstable joint (grade 2)
- Unstable joint (grade 3)
- Unable to put weight on the leg (grade 3)
Diagnosis :
The clinical diagnosis is confirmed with an MRI scan of the affected Knee.
Recommendations for treatment include the following:
- Grade I: Rest, ice compression and elevation are very important. Short-term use of crutches may be indicated, with weight-bearing as tolerated.
- Grade II: A short-hinged brace that blocks 20° to 30° of terminal extension but allows full flexion should be used. Knee closed chain exercises for strengthening of Knee muscles are indicated.
- Grade III: The patient initially should be non–weight-bearing (NWB) on the affected lower extremity. A hinged braced should be used with gradual progression to full weight-bearing (FWB) over 4 weeks. Grade III injuries may require 8-12 weeks to heal.
- Any type of Knee Ligament Injury to the Medial Collateral Ligament should be treated with early range of motion (ROM) and strengthening of the musculature that stabilizes the Knee Joint.
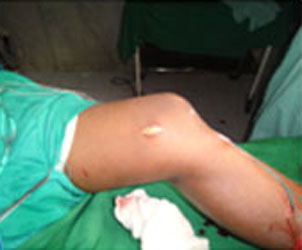
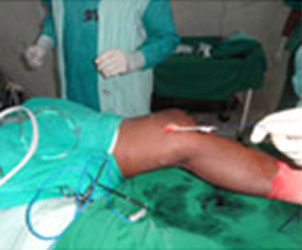
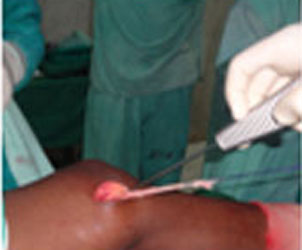
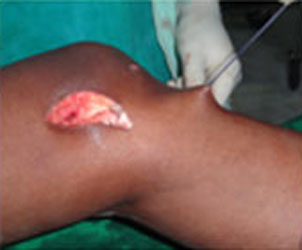
Surgical Management:
The only two indications of MCL Repair are:
1) Complete MCL Tear coexisting with other ligament injuries.
2) MCL Tears that have healed with residual laxity (looseness), causing persistent instability of the Knee.
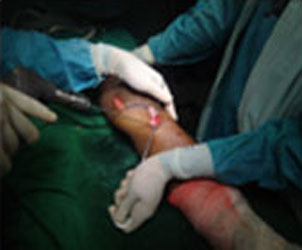
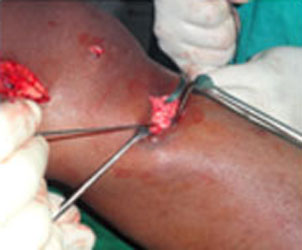
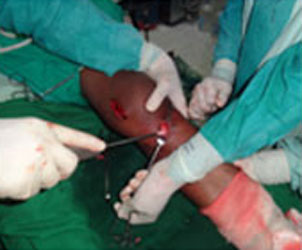
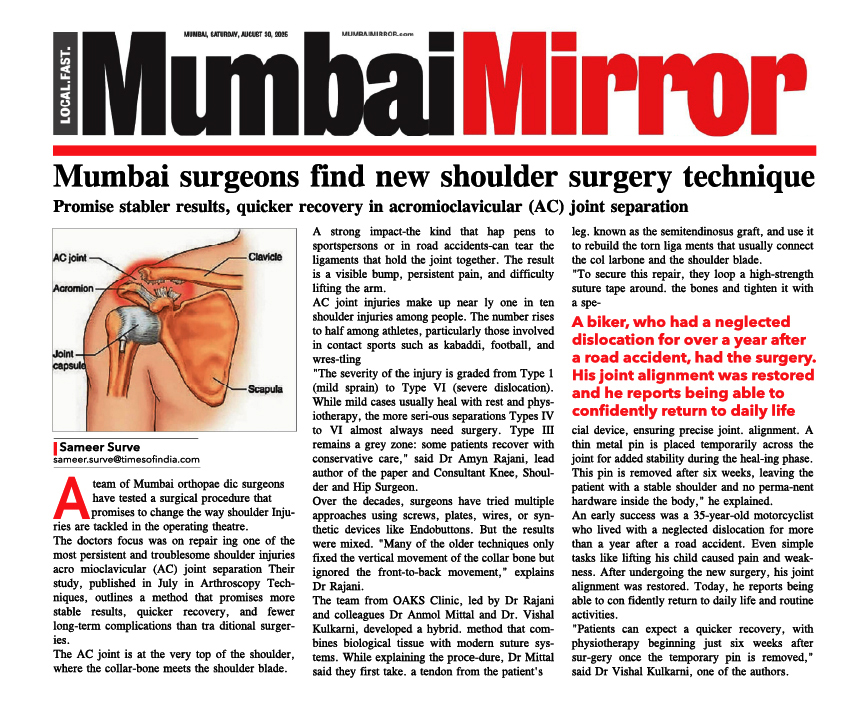
The surgery for MCL is an open surgery.
Primary end-to-end repair is possible if the MCL Reconstruction Surgery is done less than 3 weeks after injury. MCL surgery is done via an open incision on the inner portion of the Knee. If the operation is done in the acute setting (< 3 weeks after injury), primary repair of the torn ligament is possible. Bony avulsions of the ligament are fixed to the bone by suture anchor.
In cases of chronic MCL laxity and instability, MCL Reconstruction Surgery is often necessary. Hence, a new MCL is prepared from an autograft tissue. The new ligament is then placed over the top of the old MCL and secured to femur and tibia with fixation devices.
Steps of MCL Reconstruction: