PLC Tear & PLC Reconstruction
The Posterior-Lateral Corner (PLC) is a part of the knee joint that is located at the outside (lateral) back (posterior) of the knee, comprising of many ligaments, tendons, and soft tissues. These structures overlap to attach to various structures, and help to maintain the static and dynamic stability of the posterior lateral knee. They help in preventing too much rotational and sideways movement at the knee, as well as protect from over extending the knee.
The various structures in the PLC are the popliteus tendon, popliteofibular ligament, lateral collateral ligament, posterolateral joint capsule, oblique popliteal ligament, popliteus muscle, illiotibial band, biceps femoris, and the lateral gastrocnemius tendon.
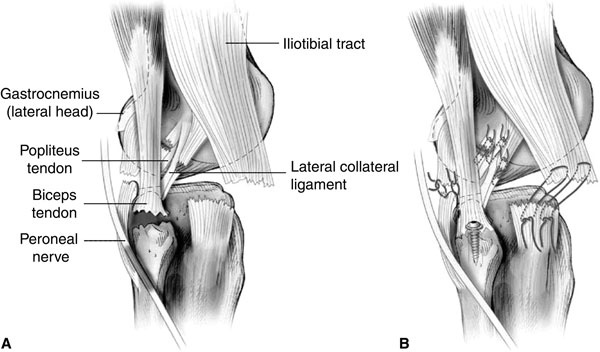
Tears of the Posterolateral Corner:
Posterolateral force directed to the inside of the Knee, Knee hyperextension, or excessive knee rotation when the Knee is on the ground and partially bent are the causes of injury to the PLC. They frequently occur with other ligament injuries, such as an Anterior Cruciate Ligament Tear or Posterior Cruciate Ligament Tear.
Symptoms:
Patients often complain of knee joint pain and instability at the joint. Bruising over the outer aspect of thigh may also be seen.

Clinical Tests :
Gait Exam
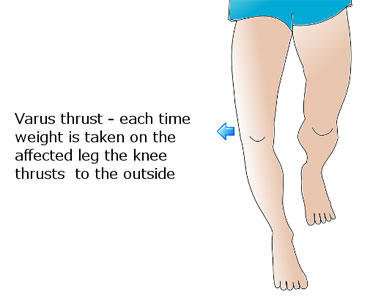
- Varus Thrust or Hyperextension Thrust
Varus Stress Test
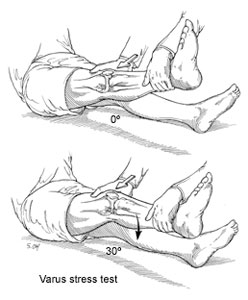
- Varus laxity at 0° indicates both LCL & cruciate (ACL or PCL) injury.
- Varus laxity at 30° indicates LCL injury.
Dial Test
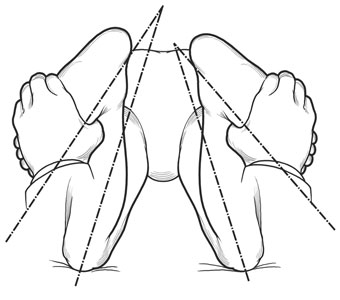
- More than 10° of external rotation asymmetry between both lower limbs at 30° of flexion only is consistent with isolated Posterior-Lateral Corner Injury.
- More than10° of external rotation asymmetry at 30° & 90° of flexion of the knee consistent with both PLC and PCL injury.
External Rotation Recurvatum
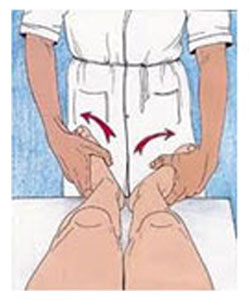
- Positive when lower leg falls into external rotation and recurvatum when leg suspended by toes in supine patient.
Posterolateral Drawer Test
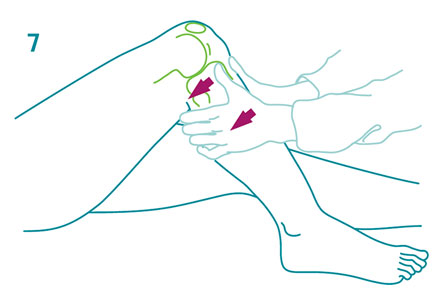
This is performed with the hip flexed 45°, Knee flexed 80°, and foot is ER 15°. A combined posterior drawer and external rotation force is then applied to the knee to assess for an increase in Posterolateral translation (lateral tibia externally rotates elative to lateral femoral condyle).
Reverse Pivot Shift Test
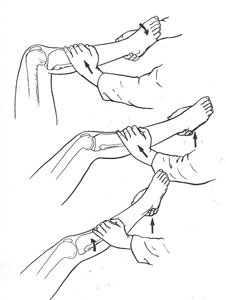
- Knee positioned at 90° and external rotation and valgus force applied to tibia
- As the knee is extended tibia reduces with a palpable clunk.
- Tibia reduces from a posterior subluxed position at ~20° of flexion to a reduced position in full extension (reduction force from IT band transitioning from a flexor to an extensor of the Knee).
- Peroneal nerve injury.
- Altered sensation to dorsum of foot and weak ankle dorsiflexion.
- Approximately 25% of patients have peroneal nerve dysfunction.
Management
Conservative Treatment :
- Immobilize knee in full extension with protected weight bearing for ~2 weeks.
This is usually done in isolated Posterior-Lateral Corner Grade I or II injuries. This is usually followed by progressive functional rehabilitation focusing on quad strengthening with return to sports in 8 weeks.
Surgical Management
PLC Repair :
This can be done only when there is an acute (within 2 weeks) and isolated injury of the Posterior-Lateral Corner with bony or soft tissue avulsion.
PLC Reconstruction:
It is done for most Grade III isolated injuries as well as Multiligament injuries.
The goal is to reconstruct LCL and the popliteofibular ligament using a free tendon graft (semitendinosus or achilles).
There are two types of reconstruction techniques as follows :
Fibular-based reconstruction (Larson)
In this the hamstring graft passed through bone tunnel in fibular head and the two limbs of the graft are crossed to create figure-of-eight and fixed to lateral femur.
Trans-tibial double-bundle reconstruction
Split achilles tendon is fixed to isometric point of the femoral epicondyle.
One limb is fixed to the fibular head with a bone tunnel and transosseous sutures to reconstruct the LCL.
The second limb is brought through the posterior tibia to reconstruct the popliteofibular ligament.
Rehabilitation:
- 4 weeks of post-operation cast controls leg ER better than knee brace.
- Gradual mobilization is then begun.
Steps of Larson Procedure: